A Mother’s Mission to Save Her Son
By Glenda Swinbourn, LRG Contributor

In this article, Mom Glenda Swinbourn of Australia shares the story of her son Mitchell, a 13-year old with Carney-Stratakis Dyad. It is for patients like Mitch that the Pediatric & SDH-Deficient GIST Consortium was founded.
Mitchell has faced many battles in his young life, even prior to birth, including being diagnosed with high-functioning autism. Little did we realise, our hardest journey was yet to come.
Mitch’s GIST journey began with a troubling set of symptoms over several months, that began with uncontrollable vomiting daily, a small breast lump, and ongoing severe headaches for which he was hospitalized in April of 2015.
At that time, we requested blood and urine tests and were told, “If you don’t hear back from us, you know everything is ok.” Nothing was heard. My husband’s brother had been diagnosed with paragangliomas years before, and I knew the vomiting and headaches were symptoms he had suffered. There was mention of a potential hereditary risk after his diagnosis, but that was never explained to us as a serious risk.
Our GP diagnosed anxiety as the cause of the vomiting due to Mitchell’s autism, and advised he take a week off school. I wasn’t convinced, especially when days later Mitch begin vomiting blood. I urged the doctors to check last April’s blood results to confirm everything was ok but was told they couldn’t be located.
When I discussed my concerns regarding our family history of paragangliomas, there was always a blank stare. We were sent home with medication to hopefully help Mitchell’s stomach lining settle. Two days later, undeterred and desperate, I went back to Emergency Department (ED) and saw another doctor. I poured out my concerns, and he ordered x-rays.
Still unable to find the prior blood results, the doctor diagnosed constipation. Mitch had an enema and was sent home with a seven-day course of medication. What I didn’t know until months after the first tumour removal was that this doctor had identified a mass in the stomach, but knowing Mitchell had autism, decided it was a mass of hair Mitchell had eaten.
To this day my husband and I can never understand why the doctor made that assumption and that he never even asked me if Mitchell tended to eat strange things. When we saw Mitchell’s paediatrician, I again poured out his history and my concerns, asked her to find the results from the hospital for me, which she did. I sat there in her office with Mitch building with Legos at a table next to me.
The paediatrician got through to the head of pathology and after a minute or two said those words I will never forget “So, the parents should have been informed…” and began writing figures. Adrenaline was the first one noted and the number was in the thousands.
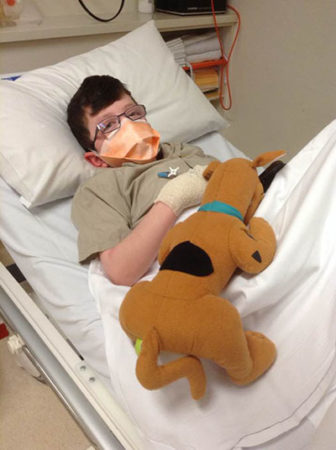 I knew it suggested a paraganglioma. I looked at Mitchell and felt panic rising within me. Mitchell’s paediatrician told me she would refer us to an endocrinologist and we would need to wait for them to get in contact.
I knew it suggested a paraganglioma. I looked at Mitchell and felt panic rising within me. Mitchell’s paediatrician told me she would refer us to an endocrinologist and we would need to wait for them to get in contact.
That night Mitchell woke with a severely swollen abdomen and I rushed him to hospital. I told them about our results and that prior blood tests potentially indicated a paraganglioma. I told them I was scared and that something was terribly wrong. A senior doctor came to examine Mitchell, and told me to stop the constipation medication, that it had done its job and Mitchell no longer needed it. I told him Mitchell had not been passing much at all, to which he replied, “It’s possible he hasn’t passed it yet – perhaps continue with the seven-day plan.” I glared angrily at him and told him this was our third time to ED in one and a half weeks and I wanted answers, real answers. After relating the risks of more radiation, he agreed to order an x-ray. The junior doctor later told us his x-ray showed no constipation issues, so we could stop his medication and we were free to leave.
I felt rage coursing through me; it took every bit of self-control I had not to scream. I should have. I should have refused to leave, ordered them to get another doctor, and made a scene. But I didn’t, I did what they told me to do and I took Mitchell home. It went against my upbringing to stand up to doctors, but I didn’t believe them. I felt betrayed and knew if I was right, Mitchell was quite literally a ticking time bomb. If a paraganglioma was there it could secrete enough adrenaline to cause a stroke or kill Mitchell outright by causing a heart attack. I was desperate and so very scared.
I received a call from an endocrinologist who reviewed Mitchell’s case and apologized for the trauma our family had endured. She told me the symptoms and tests indicated that Mitchell did have a paraganglioma. I felt so many emotions flooding through me: relief that I was being taken seriously, overwhelming grief, anger, fear and exhaustion.
Diagnosis Confirmed
A 24-hour urine screen performed twice by the endocrinologist confirmed I was right, as it gave all the signs a secreting paraganglioma was present. An MIBG scan identified a mass in his abdomen and Mitch underwent two weeks of blockers to lower his blood pressure.
Without blockers, the para had the potential to cause an adrenaline surge during surgery, enough to awaken Mitchell and cause a stroke or even death.
During the two-week initial wait in hospital undergoing the blockers, Mitchell continued to vomit. During an ultrasound, a second tumour was identified in Mitchell’s stomach. Logically we assumed it was another para and but after its removal, we were told it was potentially a GIST. I don’t think my husband, or I will ever forget the excitement in the well-meaning oncologist’s voice. “This would be the first GIST ever diagnosed at the hospital. Mitchell was an extremely rare case; doctors were lucky to ever come across this cancer in their lifetime”. The enthusiasm was not shared by us. We felt afraid and concerned that due to this rarity, we again, had no cure or protocol treatment. We didn’t understand how we could be battling two types of rare tumours at the same time.
The Family Connection
 Research led me to Carney-Stratakis Dyad – paras and GIST, caused by the SDHB mutation and it was therefore no surprise when suggestions were made that this was the diagnosis. We realized that for Mitch to have this mutation, my husband must possess it and therefore our two other boys could also be at risk. Mitchell’s tests came back three months later, following his first tumour removal, positive for SDHB mutation. This then enabled my husband to be tested. With the positive result our other two sons were tested. Our youngest son is positive and our oldest is not. This meant my husband and youngest son need to be screened on a regular basis.
Research led me to Carney-Stratakis Dyad – paras and GIST, caused by the SDHB mutation and it was therefore no surprise when suggestions were made that this was the diagnosis. We realized that for Mitch to have this mutation, my husband must possess it and therefore our two other boys could also be at risk. Mitchell’s tests came back three months later, following his first tumour removal, positive for SDHB mutation. This then enabled my husband to be tested. With the positive result our other two sons were tested. Our youngest son is positive and our oldest is not. This meant my husband and youngest son need to be screened on a regular basis.
The surgeons claimed that Mitchell’s GIST had been removed with clear margins, but that the paraganglioma which had attached to the abdominal aorta had also grown into the vena cava, so it was regarded as an incomplete resection. With regular MRI’s, the occasional CT and PET scans, things were clear until May 2016, when two new lesions were discovered in Mitchell’s liver.
Our oncologist, Dr. Rishi Kotecha from Perth, reached out to experts around the world to find the best treatment options. Dr. Kotecha felt Dr. Lee Helman and Dr. Katherine Janeway’s suggestion to use the tyrosine kinase inhibitor, Pazopanib, was the best course of action. I knew there was limited evidence to support the use of these drugs and quite frankly, my husband and I were terrified of what the drug might do to Mitch’s little body. I researched extensively and emailed GIST support groups for information on their own experiences.
In the end, we opted for radiofrequency ablation. It was at this time Mitch became extremely ill and it took around a week for doctors to find the cause. Ultimately, he underwent a second laparotomy at the beginning of August to rectify bowel adhesions which had developed as a result of his first laparotomy. It was a difficult recovery but at the end of August, when Mitch was strong enough, he underwent a radiofrequency ablation procedure to destroy the two liver lesions.
At the time the ablation was performed a biopsy was also taken, and although we suspected GIST, we also realized the possibility of the tumour being a paraganglioma. Knowing that a biopsy was considered unsafe if the tumour was a para, we refused a biopsy to be performed on their discovery. It was with great angst we allowed them to take the tissue simultaneously while the burning occurred. We needed to know with certainty what we were dealing with. The results confirmed our suspicions that GIST was indeed our diagnosis.
In a follow-up 12 weeks later, we were devastated to discover Mitchell had three new lesions in his liver and in December 2016, he underwent a second radiofrequency ablation procedure. At the next 12-week follow-up after this procedure we were again shattered to find Mitchell now had a total of five new lesions present in his liver. Ablation was now considered unfeasible due to positioning of tumours and current damage to the liver. In the beginning of 2017, it was decided that our best course of action would be to place Mitchell on Pazopanib.
 Thankfully, the only side effects our little boy encountered was a change in his hair colour and constant nasal congestion.
Thankfully, the only side effects our little boy encountered was a change in his hair colour and constant nasal congestion.
In July of 2017, our family undertook a huge journey to travel from Perth in Western Australia to the National Institutes of Health in the U.S., to take part in their annual Pediatric and Wild-Type GIST Clinic. Mitchell was examined by top experts and our whole family provided DNA, something which we felt was extremely important, not only for Mitch, but with the hope of helping others already affected and those yet to be diagnosed.
Over a year, Mitchell’s five liver lesions continued to grow, and in February, Mitch was placed in the PRISM Trial at Princess Margaret Hospital. He was hospitalised to undergo a fine needle biopsy which would use tumour tissue with the aim of individualizing treatment based on the specific genetic make-up of his tumours. The following month, after yet another MRI, we were informed not only had the biopsy removed unviable tissue, but that all his tumours had grown significantly, plus he now had a sixth lesion close to the outer surface of the liver.
After much discussion, we ceased Mitchell’s medication and in April, a Sydney paediatric liver specialist flew to Perth and conducted yet another laparotomy to remove the new lesion. Unfortunately, the remaining lesions were deemed inoperable, due, not only their location, but the inability for the remaining liver to function viably. We were very relieved when around six weeks later we were told the painful procedure had been successful and the tissue was viable – thus allowing us to proceed in the trial.
The follow up in July indicated the five remaining tumours had again grown significantly and heartbreakingly, another two lesions had arisen, taking his total to seven active lesions. After the results of the first part of the trial were revealed. we were advised to try a second TKI called Regorafenib. This drug proved to be harsher and resulted in Mitch developing terrible foot pain with severe blistering and peeling.
As with the Pazopanib, the results of Mitchell’s latest MRI showed once again a failure to achieve stability in his tumours, instead seeing a continued increase. We were also able to distinguish that the growth rate had slowed, and we made the joint decision to lower the dosage and hope the side effects would be reduced. Mitchell started the lower dose of Regorafenib over the last few days. We are holding our breath and waiting, hoping our little boy, who has suffered so much, will suffer as little as possible for the time we have left with him.
 Our family lost my husband’s brother in September 2016 due to metastatic paraganglioma and pheochromocytoma caused by the SDHB mutation. He was 36, and even though ill, he was a great support for our family as we battled our own rareness. Our family lost my Dad in 2017 and my Mum this past August.
Our family lost my husband’s brother in September 2016 due to metastatic paraganglioma and pheochromocytoma caused by the SDHB mutation. He was 36, and even though ill, he was a great support for our family as we battled our own rareness. Our family lost my Dad in 2017 and my Mum this past August.
Death seems ever present, and anxiety, depression, and grief have impacted my life heavily over these last few years. I continue to find all my strength in this little boy, who has endured so much pain, and continues to smile and fight this relentless disease. Watching a child fight cancer is unbelievably painful; watching a child fight an incurable cancer is soul-destroying.
We try to live one day at a time, and I continue to research trials, still hoping that tomorrow we have options to give our little boy as much time as possible. If you would like to follow Mitchell’s story, he has a Facebook page, Team Mitchell, www.facebook.com/myrarecancer.



